Fall 2023 Featured Items
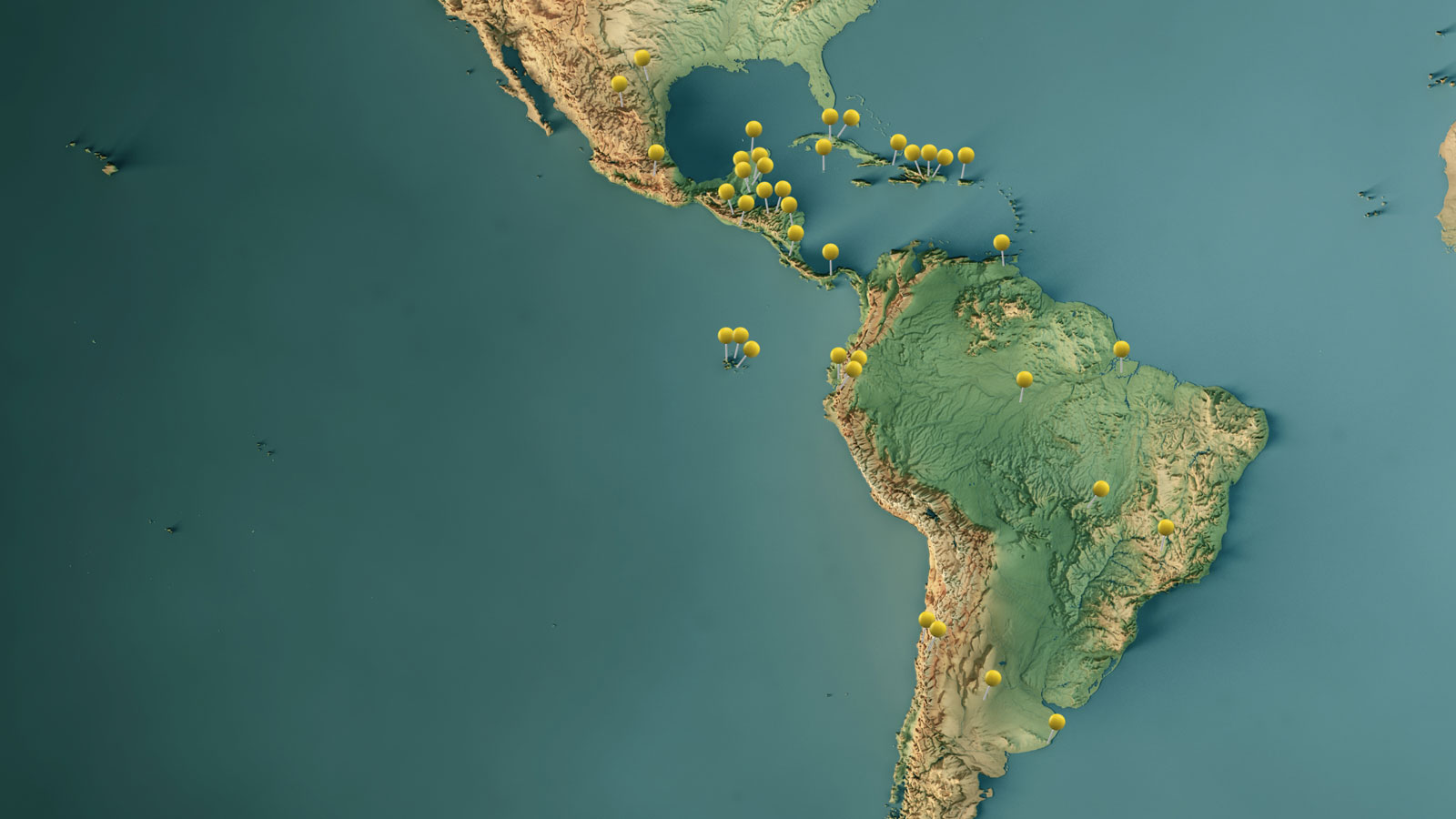
The College of Arts & Sciences is playing a vital role in advancing the University's impact across the Americas
A look at what kind of research and collaborations A&S faculty are working on in Latin America
Baylor’s new transmission electron microscope opens the doors to important research
Two history professors are using their heritage to engage students
A popular program created to foster writing and research among Baylor’s female faculty is expanding its focus
Humanities students are using a new minor to gain better insight into the natural world
The new aerospace studies minor prepares students for aviation careers
Baylor’s new ethnic studies minor aims to foster a sense of belonging and inclusion
Fall 2023 Departments
In this issue we are devoting space to inform our readers about what kind of research and collaborations A&S faculty are working on in Latin America, as we pursue the goals of the Baylor University strategic plan.
Updates on faculty, staff, students and alumni.
As 2023 nears its end, the College of Arts & Sciences is completing a yearlong celebration of this magazine’s 10th anniversary.
Greg Lewallen, a senior lecturer in art and art history, has spent the past 10 years making more than 100 drawings of insects such as this in Latin America